Arthritis Myths and Facts: 9 Common Misconceptions You Should Stop Believing

Arthritis myths and facts are easy to confuse especially when bad information spreads faster than good science. You have probably heard that arthritis is just part of getting old, or that exercising with joint pain makes things worse, or that surgery is the only real fix. These ideas are everywhere. And they are mostly wrong.
In the United Kingdom alone, millions live with arthritis making it one of the leading causes of disability in the country. More than half are working-age adults. This is not a condition limited to the elderly. Arthritis myths and facts clearly show It affects professionals, parents, athletes, and children across London and beyond.
Yet the arthritis myths and facts keep circulating. And when people believe them, they delay treatment, avoid movement, or make decisions that worsen their condition including their knee pain.
Arthritis myths and facts 1: Arthritis Only Affects Older People
Fact: Arthritis in Young Adults Is Far More Common Than Most People Realise
This is probably the most widespread misconception in Arthritis myths and facts. The mental image of arthritis, a slow-moving elderly person with swollen knuckles is outdated and misleading. More than 50% of arthritis cases in the UK occur in adults under 65.
Conditions like rheumatoid arthritis frequently develop between the ages of 30 and 50. Arthritis myths and facts prove that age is a risk factor, not a rule. Psoriatic arthritis, gout, and ankylosing spondylitis also affect people well below retirement age. Arthritis in young adults is not rare; it is underdiagnosed, largely because neither the patient nor their doctor thinks to look for it.

Why Does This Myth Persist?
Osteoarthritis, the most common type, does tend to develop gradually over time which leads people to associate all arthritis with aging. But osteoarthritis is just one of over 100 types. Many others are driven by the immune system, genetics, or a previous joint injury. None of those require you to be a certain age.
Being young does not protect you. Getting older does not guarantee you will develop arthritis. Age is a risk factor, not a rule.
Myth 2: Children Cannot Get Arthritis
Fact: Juvenile Idiopathic Arthritis Affects Around 300,000 Children in the UK
Arthritis myths and facts also debunk the belief that children cannot get arthritis. Juvenile Idiopathic Arthritis (JIA) is real and serious and the most common form affecting those under 16. According to the Cleveland Clinic, approximately one in every 1,000 children in the US develops it.
JIA causes the same hallmark symptoms as adult arthritis: joint pain, swelling, stiffness, and reduced range of motion. Left untreated, it can cause permanent joint damage and affect normal physical development.
How Early Can It Start?
Some children are diagnosed as young as 12 months old. The condition does not wait for a child to hit a certain age or growth stage. And unlike a minor sports injury, it does not simply resolve on its own.

Early diagnosis and consistent treatment dramatically improve outcomes. With the right care, many children with JIA go on to live fully active lives. Without it, the damage done in those early years is often irreversible.
Myth 3: All Joint Pain Including Knee Pain Is Arthritis
Fact: All Joint Pain Is Not Arthritis, and Getting the Diagnosis Right Matters
This myth causes real harm. Arthritis myths and facts highlight why correct diagnosis is crucial. When someone assumes their knee pain is arthritis, they may self-treat for a condition they do not actually have while the real problem continues to develop untreated.
Knee pain, in particular, is one of the most common complaints in both younger and older adults. But it has a wide range of possible causes beyond arthritis.
Conditions That Mimic Arthritis in the Knee
- Tendonitis — inflammation of the tendons around the joint
- Bursitis — inflammation of the fluid-filled sacs that cushion the joint
- Ligament sprains or cartilage tears — common from physical activity or injury
- Patellofemoral syndrome — pain behind the kneecap from overuse or poor alignment
- Baker’s cyst — fluid build-up behind the knee causing swelling and stiffness
Each of these requires a different treatment approach. Treating a Baker’s cyst like rheumatoid arthritis or vice versa is not just ineffective. It can delay the right care for months.
A rheumatologist can assess your specific symptom pattern, run appropriate tests, and confirm what is actually causing the pain. That step matters far more than most people think.
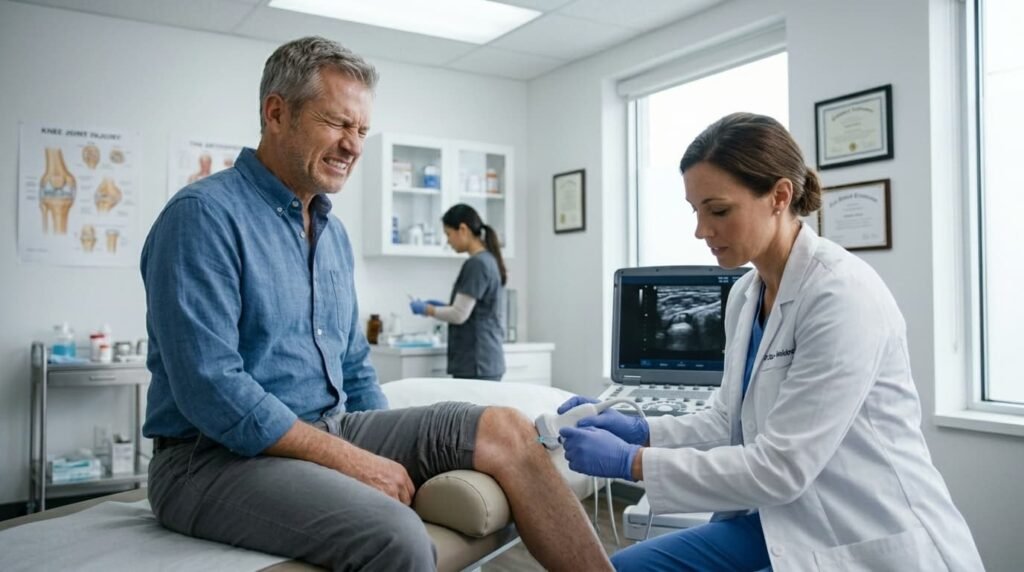
Myth 4: You Should Wait and See If Joint Pain Resolves on Its Own
Fact: Early Diagnosis Arthritis Treatment Prevents Long-Term Damage
Joint pain that comes and goes might feel like something to monitor. Arthritis myths and facts strongly recommend early diagnosis. And occasionally, a minor ache after a long hike really does resolve on its own. But persistent or unexplained joint pain is a different matter entirely.
When you delay diagnosis for inflammatory arthritis like rheumatoid arthritis you give the disease more time to cause damage. And that damage is not limited to the joints. Without treatment, rheumatoid arthritis can affect the skin, eyes, lungs, blood vessels, and heart.
When Should You See a Doctor for Joint Pain?
- Pain, swelling, or stiffness that lasts longer than a few days without a clear cause
- Symptoms that keep returning even after rest
- Morning stiffness in the knee or other joints that takes more than 30 minutes to ease
- Joint pain that makes everyday tasks walking, climbing stairs, getting up from a chair harder than normal
- Visible swelling or warmth around a joint
None of these are reasons to panic. But all of them are reasons to see a doctor. The earlier arthritis is identified, the more options exist to manage it and slow its progression.
Myth 5: Exercising Will Make Arthritis Worse
Fact: Exercise for Arthritis Patients Is One of the Most Effective Treatments Available
This arthritis miths and facts keeps people sitting still when movement is exactly what their joints need. Joint pain makes exercise feel risky. But inactivity is often more harmful than gentle, appropriate movement.
Regular exercise strengthens the muscles that support and stabilise joints. Stronger supporting muscles mean less direct load on the joint surface. For knee arthritis specifically, building quadricep and hamstring strength is one of the most effective ways to reduce daily pain and improve function.
What Types of Exercise Work Best for Arthritis Patients?
- Swimming and water aerobics — low impact, full range of motion, easy on the knee
- Cycling — strengthens the knee without high-impact loading
- Walking — maintains mobility and supports cardiovascular health
- Targeted physiotherapy exercises — prescribed specifically for your joint and arthritis type
- Gentle yoga or stretching — improves flexibility and reduces stiffness
During a severe flare, resting the affected joint makes sense. But outside of those periods, staying active with guidance from a physiotherapist is one of the most valuable things an arthritis patient can do. The goal is not to push through pain. It is to maintain function, strength, and mobility in a way that is appropriate and sustainable.
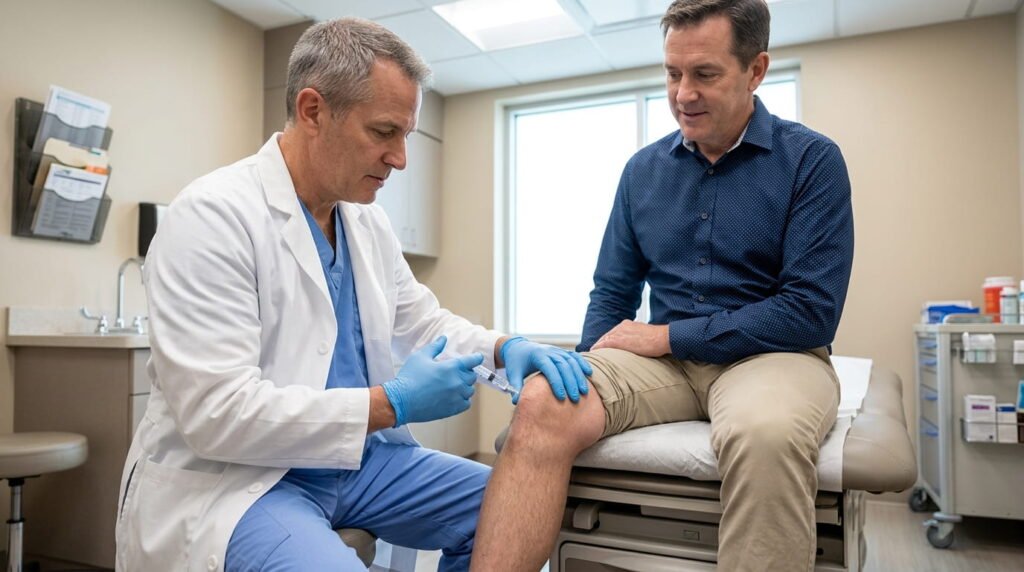
Myth 6: Injections Damage Joint Cartilage
Fact: Cortisone, Hyaluronic Acid, and Arthrosamid Injections Are Safe Options When Used Correctly
Patients often arrive at clinics having already decided against injections because they have heard the treatments damage cartilage or cause long-term harm. This is not supported by the evidence when injections are used appropriately.
Cortisone Injections
Cortisone is an anti-inflammatory steroid that reduces swelling and pain in the joint. It works quickly and provides meaningful relief for moderate to severe arthritis including knee pain. Arthritis myths and facts clear the confusion around injections. The key is spacing: cortisone injections should generally be at least three months apart. Overuse does carry some risk, but used correctly, they are a legitimate and effective tool.
Hyaluronic Acid Injections
Hyaluronic acid occurs naturally in joint fluid and helps lubricate and cushion the joint. In osteoarthritis, this fluid degrades over time. Hyaluronic acid injections help restore some of that cushioning particularly in the knee. Arthritis myths and facts show many patients manage well without surgery. They can typically be given every six months and are well-tolerated by most patients.
Arthosamid Injections
Arthosamid is a newer injectable option developed specifically for knee osteoarthritis. It is a water-based polyacrylamide hydrogel that integrates into the soft tissue inside the knee joint, providing cushioning and sustained pain relief. Unlike cortisone, it is not a steroid. Unlike hyaluronic acid, it is designed to remain in the joint for a longer period. Early clinical evidence suggests it can offer meaningful, long-lasting pain reduction for patients who have not found adequate relief with other non-surgical options. A specialist consultation is needed to confirm whether it is suitable for your specific case.
None of these injections are cures. But each offers a real, evidence-based way to manage arthritis particularly knee arthritis without surgery. Arthritis myths and facts they work best as part of a broader plan that includes exercise, weight management, and appropriate medication.
Myth 7: Surgery Is the Only Real Treatment for Osteoarthritis
Fact: Effective Arthritis Treatment Without Surgery Exists for Most Patients
Arthritis myths and facts is progressive. For some people, joint replacement eventually becomes the right decision. But “eventually” covers a lot of ground and for most people, non-surgical management works well for years.
The majority of people with osteoarthritis manage their condition without surgery for a significant portion of their lives. The key is starting appropriate treatment early and adjusting it as the condition evolves.
Non-Surgical Treatment Options for Knee Arthritis
- Physiotherapy — builds strength around the knee, improves mobility, reduces pain
- NSAIDs — reduce pain and inflammation, available in oral and topical forms
- Cortisone or hyaluronic acid injections — provide targeted relief in specific joints
- Arthosamid injection — newer hydrogel option for knee osteoarthritis with longer-lasting cushioning effect
- Weight management — reduces mechanical load on weight-bearing joints like the knee
- Hot and cold therapy — heat eases morning stiffness, cold reduces post-activity swelling
- Braces and orthotics — reduce joint stress and improve alignment during daily activity
For knee arthritis specifically, the combination of physiotherapy, weight management, and targeted injections gives many patients years of manageable, functional life without surgery. Surgery remains an option when these approaches no longer provide adequate relief — but it should be a considered last step, not a first assumption.
Myth 8: Dietary Changes Can Cure Arthritis
Fact: An Anti-Inflammatory Diet Helps Manage Symptoms — But Cannot Reverse the Condition
Diet and arthritis sit in a space where Arthritis myths and facts run in both directions. Some insist food has nothing to do with joint health. Others believe the right combination of ingredients will heal them completely. Neither position is accurate.

No diet cures arthritis. The structural joint damage caused by osteoarthritis cannot be reversed by what you eat. And while certain foods can reduce systemic inflammation, they do not eliminate the underlying condition.
What an Anti-Inflammatory Diet Actually Does
- Omega-3 fatty acids (salmon, sardines, flaxseed, walnuts) — reduce inflammation throughout the body
- Antioxidant-rich foods (berries, leafy greens, broccoli) — support the body’s ability to manage oxidative stress
- Whole grains and legumes — help maintain a healthy weight, reducing load on joints
- Foods to limit — processed foods, trans fats, and excess sugar promote inflammation and worsen symptoms
Managing body weight through diet is perhaps the most direct food-related benefit for knee arthritis. Every extra kilogram of body weight adds around four kilograms of additional force on the knee joint. Reducing that load through diet and light activity can meaningfully reduce daily pain without a single prescription.
Use diet as a supportive strategy, not a replacement for treatment. It works best alongside medical care not instead of it.
Myth 9: Arthritis Symptoms Cannot Be Improved
Fact: With the Right Treatment, Most Arthritis Patients See Meaningful Improvement
This is the most discouraging myth of all and one of the most damaging. When people believe nothing can help, they stop seeking help. They accept a level of pain and limitation that, in many cases, does not have to be permanent.
There is no cure for most types of arthritis. But no cure does not mean no improvement. Treatment consistently reduces pain, protects joint function, and slows disease progression and it works.
What Improvement Looks Like in Practice
- For osteoarthritis: pain medications, physiotherapy, weight management, and targeted injections often restore significant function
- For rheumatoid arthritis: disease-modifying antirheumatic drugs (DMARDs) suppress the immune response that damages joints, reducing inflammation and preventing further deterioration
- For knee arthritis specifically: a combination of strengthening exercises, appropriate injections, and orthotics can substantially reduce daily pain
Many patients who begin treatment expecting modest results are surprised by how much function they regain — the ability to walk comfortably, return to exercise, sleep through the night, or simply get up from a chair without dreading it. These are real, achievable outcomes with consistent care.

FAQ
Is arthritis only in old age, or can younger adults develop it too?
Arthritis is not age-restricted. More than half of people with arthritis in the US are under 65. Conditions like rheumatoid arthritis commonly develop between ages 30 and 50. Age increases risk but does not determine who gets arthritis.
Can children get arthritis?
Yes. Juvenile Idiopathic Arthritis (JIA) affects approximately 300,000 children in the UK and can cause joint damage if not treated early. Some children are diagnosed as young as one year old. Early treatment is essential to protect joint development.
When should I see a doctor for joint pain?
See a doctor if joint pain or swelling lasts more than a few days without explanation, keeps returning, causes morning stiffness for more than 30 minutes, or starts limiting normal activities like walking or climbing stairs. Early diagnosis leads to better outcomes.
Are cortisone, hyaluronic acid, and arthrosamid injections safe for knee arthritis?
Yes, when used appropriately. Cortisone reduces inflammation quickly and is safe with at least three months between treatments. Hyaluronic acid restores joint lubrication and can be repeated every six months. Arthosamid is a newer hydrogel designed to provide longer-lasting cushioning in the knee. All three are used as part of a non-surgical management approach and are considered safe under specialist guidance.
Can diet cure arthritis?
No. No diet cures arthritis. However, an anti-inflammatory diet rich in omega-3 fatty acids, antioxidants, and whole foods can reduce inflammation and help manage symptoms. Managing body weight through diet also directly reduces the load on knee joints, which lowers pain.
What are the best non-surgical treatment options for knee arthritis?
Effective non-surgical options include physiotherapy, NSAIDs, cortisone or hyaluronic acid injections, arthrosamid injections, weight management, hot and cold therapy, and braces or orthotics. Most patients manage knee arthritis without surgery for years with the right combination of these approaches.
Can arthritis symptoms be improved?
Yes. While most types of arthritis have no cure, symptoms can be significantly reduced with the right treatment. Osteoarthritis responds well to physiotherapy, weight management, and injections. Rheumatoid arthritis is managed with disease-modifying antirheumatic drugs (DMARDs). Many patients regain meaningful function and quality of life with consistent care.
Arthritis is one of the most misunderstood conditions of our time, yet real, evidence-based options exist from exercise and physiotherapy to targeted injections and diet. Early diagnosis is the single most important step; the sooner you are assessed, the more options remain available.
For persistent knee pain, Mr. Syed Nadeem Abbas (MBBS, MRCSEd, MSc) and his team at Knee Pain Clinic UK specialise in all forms of knee arthritis and the latest non-surgical treatments including Arthrosamid injections, hyaluronic acid therapy, and personalised physiotherapy programmes their team can help you find the right path forward. Living with arthritis does not mean accepting limitation as your permanent reality. The right care can change that.
Read more: Knee Replacement Surgery How to Know When It Is the Right Step
Read more: PRP vs Arthrosamid: Which Injection Works Better for Knee Pain?