PRP vs Arthrosamid: Which Injection Works Better for Knee Pain?

Millions of people live with chronic knee pain caused by osteoarthritis (OA). Many of them want to avoid surgery but find that standard steroid injections offer only short-lived relief.
That is exactly why the conversation around PRP vs Arthrosamid injection for knee pain has exploded in recent years. Both treatments promise meaningful, longer-lasting relief but they work in fundamentally different ways, carry different costs, and suit different types of patients.
This guide gives you a clear, evidence-based comparison so you can walk into your specialist’s office fully informed.
Before diving into the details, it helps to understand what each treatment is actually doing inside your knee joint.One uses your own biology to trigger repair; the other uses a synthetic gel to physically rebuild the joint environment. Neither is a magic bullet, but each can be transformative for the right patient.
Understanding PRP Therapy for Knee Osteoarthritis
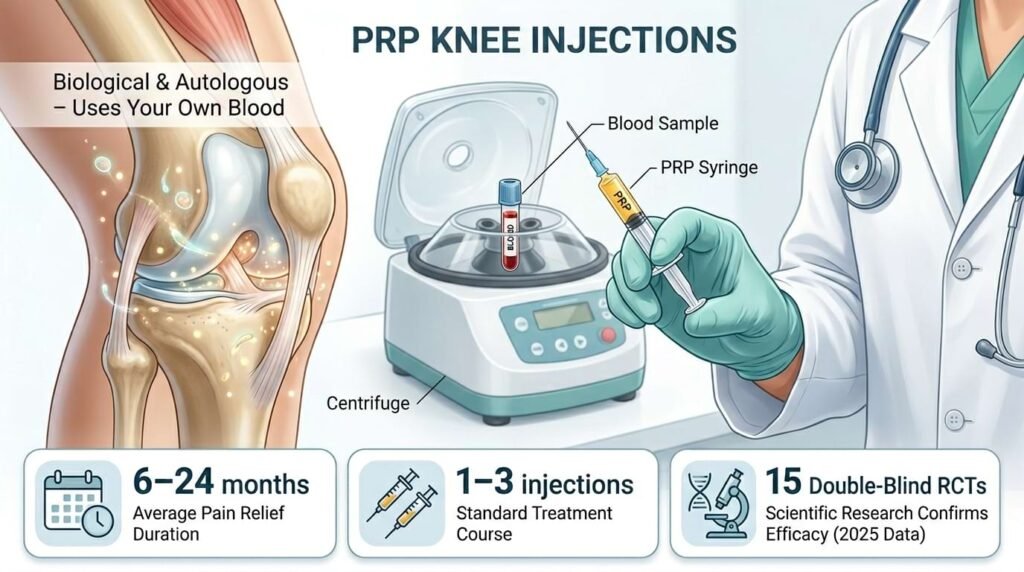
Platelet-rich plasma (PRP) therapy starts with a simple blood draw. A clinician takes a small vial of your blood and spins it in a centrifuge to separate and concentrate the platelets.
That concentrated plasma packed with growth factors like PDGF, TGF-β, and VEGF goes directly into the knee joint, typically under ultrasound guidance to ensure precise placement.
The growth factors release into the synovial fluid and work to reduce inflammation, modulate the immune response, and create a more favourable environment for tissue repair. PRP does not regenerate lost cartilage, but it can slow the inflammatory cascade that drives OA pain and stiffness.
What the Research Shows About PRP Duration
A 2025 meta-analysis of 15 double-blind randomised controlled trials found that high-platelet PRP delivered clinically significant pain relief compared to placebo at 3, 6, and 12 months.
Low-platelet preparations, however, failed to reach the minimal clinically important difference (MCID) beyond six months. This means the concentration of platelets matters enormously and that concentration varies between clinics depending on their centrifuge protocol.
In practical terms, most patients experience relief lasting 6 to 24 months. A course typically involves one to three injections spaced several weeks apart, and patients may need a repeat course when symptoms return.
The biological, autologous nature of PRP is a genuine appeal for patients who prefer to avoid synthetic materials.
Limitations of PRP You Should Know
PRP is not a standardized product. The quality and platelet concentration can vary from patient to patient and from clinic to clinic depending on the centrifuge used (single-spin versus double-spin) and the patient’s own baseline platelet count.
This variability makes results less predictable than a clinician might like. If you are evaluating PRP vs Arthrosamid injection for knee pain, this is one of the most important differences to understand upfront.
- Results depend heavily on platelet concentration and preparation protocol
- Multiple clinic visits are required for a full course
- Repeat courses may be needed every 12–24 months
- Not universally covered by insurance or NHS funding
- Evidence on long-term outcomes (beyond 24 months) remains limited
Understanding Arthrosamid: The Single-Injection Hydrogel
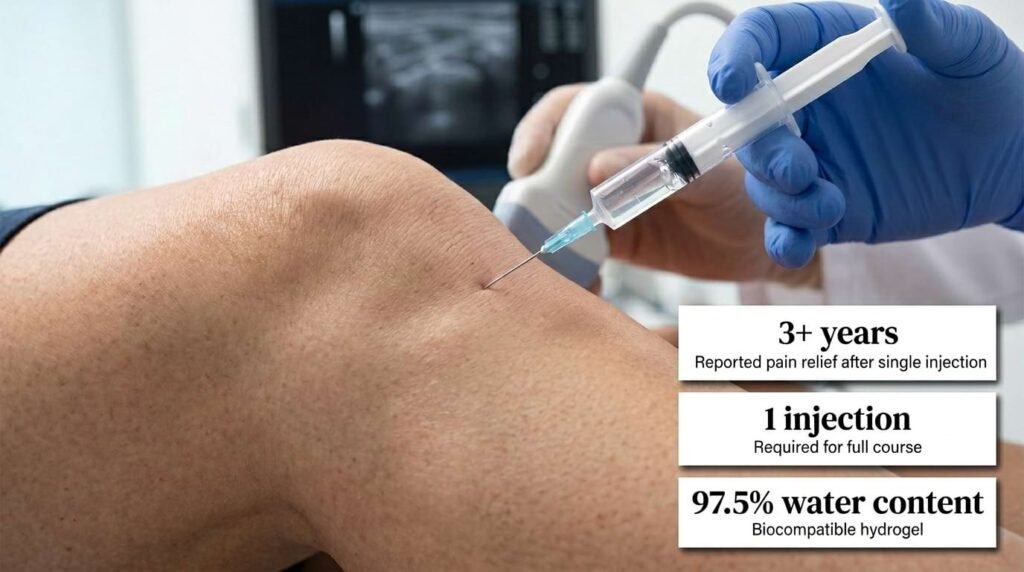
Arthrosamid is an injectable polyacrylamide hydrogel (iPAAG) with approximately 97.5% water and 2.5% cross-linked polymer. It is not a biological product.
Once a clinician injects it into the synovial cavity of the knee, it integrates directly with the synovial tissue lining the joint. Unlike temporary fillers, it does not simply sit in the joint fluid it forms a stable sub-synovial layer that persists and provides mechanical cushioning.
Animal model studies have shown histological evidence of the hydrogel persisting for up to two years. In human clinical trials, patients report meaningful, sustained pain reduction well beyond that mark.
Crucially, Arthrosamid is a one-time procedure: a single injection under local anaesthetic, performed in a clinic in under 30 minutes, with no hospital admission required.
What the Clinical Data Says About Arthrosamid Longevity
Published clinical data including the IDA and ROSA studies confirm that Arthrosamid (iPAAG) is both safe and effective for knee OA. Conference-reported follow-up data from some cohorts describe maintained pain reduction at three years and beyond after a single injection.
This makes it one of the longest-lasting intra-articular injection options currently available for non-surgical knee pain relief.
Arthrosamid does not depend on the body’s healing capacity to work. It physically changes the mechanical environment inside the joint, reducing the stress transmitted through damaged cartilage. For patients whose pain keeps returning after PRP or steroid injections, this structural approach can be a genuine game-changer.
Side Effects and Safety Profile
In a randomised controlled trial, 28.9% of patients receiving Arthrosamid reported adverse events versus 7.6% for hyaluronic acid. Importantly, all adverse events were mild or moderate predominantly local reactions like temporary injection-site pain or swelling and no serious adverse events appeared in any published study.
The overall safety profile is strong, and the treatment has received regulatory approval in multiple European countries.
PRP vs Arthrosamid Injection for Knee Pain: The Full Comparison
Now that you understand both treatments individually, let us look at how they stack up across every factor that matters to patients. This head-to-head breakdown makes the PRP vs Arthrosamid injection for knee pain decision much clearer.
| Factor | PRP Therapy | Arthrosamid |
| Duration of relief | 6–24 months | 2–3+ years |
| Sessions needed | 1–3 injections per course | Single injection |
| Predictability | Variable (protocol-dependent) | Highly consistent |
| Biological vs synthetic | Autologous (own blood) | Synthetic hydrogel |
| Side effect rate | Low (7–10%) | Moderate (28.9% mild/moderate) |
| Upfront cost | Lower per session | Higher (£2,000–£4,500+) |
| 3-year total cost | Can match or exceed Arthrosamid | One-time expense |
| Mechanism | Growth factors reduce inflammation | Hydrogel cushions and lubricates |
| Evidence quality | Multiple large RCTs | Growing robust European data |
| Surgery avoidance potential | Good for mild–moderate OA | Strong delays or prevents surgery |
How Long Does Each Knee Injection Actually Last?
Duration of relief is the number-one question patients ask when comparing PRP vs Arthrosamid injection for knee pain. The honest answer is that both treatments outperform standard corticosteroid injections, which typically provide only 6–12 weeks of meaningful relief and can damage cartilage with repeated use.

PRP’s duration depends heavily on the platelet concentration used. High-platelet PRP has demonstrated clinically relevant pain reduction up to 12 months in controlled trials. Anecdotal and open-label data suggest some patients maintain benefit for 18–24 months, particularly those with mild-to-moderate OA who receive leukocyte-poor preparations.
Arthrosamid consistently outperforms PRP on duration. Because it physically integrates into the joint lining rather than relying on biological healing, it does not degrade over time in the same way. The three-year follow-up data available from European cohorts make it the longest-documented intra-articular injection treatment currently on the market for knee osteoarthritis.
Cost of PRP vs Arthrosamid: Thinking Beyond the Upfront Price
Many patients dismiss Arthrosamid immediately when they see the upfront cost typically between £2,000 and £4,500 for a single injection in the UK, or CAD $4,000–$4,500 in Canada. By comparison, a single PRP injection may cost £400–£800, making it appear far more affordable.
But look at the three-year picture. If PRP provides 12 months of meaningful relief and you need repeat courses, a patient might receive three full PRP courses over three years equaling or exceeding the total cost of one Arthrosamid injection.
When patients frame the PRP vs Arthrosamid injection for knee pain decision in terms of total three-year spend rather than upfront cost, the gap narrows significantly.
Factor in the time cost too: multiple clinic visits for blood draws, waiting, repeat injections, and recovery days after each session add up. Arthrosamid’s single-visit model has a real-world value that a simple price comparison misses.
Who Should Choose PRP and Who Should Choose Arthrosamid?
Not every patient is a good candidate for both treatments. When you map out the ideal patient profile for each option, the choice in the PRP vs Arthrosamid injection for knee pain debate becomes much more personalised and intuitive.

Choose PRP if you:
- Have mild to moderate knee OA (Kellgren-Lawrence Grade I–III)
- Prefer a biological, autologous approach with no synthetic materials
- Have upfront cost as your primary concern
- Are comfortable attending multiple clinic visits
- Want a well-researched option with a large body of RCT data
- Have OA associated with inflammation and tissue damage that growth factors could target
Choose Arthrosamid if you:
- Need longer-lasting relief from a single treatment
- Found PRP, steroid, or hyaluronic acid results short-lived
- Are seeking to delay or avoid knee replacement surgery
- Value predictability and consistency of outcome most
- Have a busy schedule and cannot commit to repeat visits
- Want a structurally supportive treatment, not just anti-inflammatory relief
There is no single correct answer. Your specialist will consider your OA grade on imaging, your BMI, your response to previous treatments, and your personal priorities before recommending one approach over the other. Direct head-to-head trials comparing the two treatments are still limited, so clinical judgement remains essential.
What Happens After Each Injection: Recovery and Rehabilitation
Recovery is an often-overlooked factor in the PRP vs Arthrosamid injection for knee pain comparison, yet it matters enormously for working patients and active individuals.
After PRP Therapy
Most patients experience a short flare of increased knee pain and swelling in the 24–72 hours after a PRP injection. This is a normal biological response as the growth factors activate an inflammatory cascade that eventually leads to resolution and repair.
Clinicians typically advise patients to rest the joint for 48 hours, avoid anti-inflammatory medications like ibuprofen for up to a week (as they blunt the PRP effect), and begin gentle physiotherapy after the flare settles.
Some patients can return to light activity within 3–5 days. Strenuous sport or high-impact exercise should wait 4–6 weeks. Because PRP typically involves a course of injections, patients go through this recovery cycle multiple times, which can feel disruptive for those with demanding schedules.
After Arthrosamid Injection
Post-Arthrosamid recovery is generally more straightforward. The hydrogel does not trigger the same inflammatory response as PRP. Most patients experience mild injection-site discomfort for a few days and can resume normal, low-impact daily activity within a week.
Clinicians recommend avoiding strenuous activity for 2–4 weeks to allow the hydrogel to integrate fully with the synovial tissue. Because it is a one-time procedure, patients go through this recovery phase only once.
Combining PRP and Arthrosamid: Is It Possible?
Some patients ask whether they can receive both treatments. Emerging research explores PRP combined with hyaluronic acid (PRP+HA), which shows promising results in multiple meta-analyses producing superior WOMAC and VAS pain scores at 12 months compared to either treatment alone.
However, directly combining PRP with Arthrosamid is not yet standard practice and has not been studied in any published trial.

What is increasingly common in specialist practice is using PRP as a first-line option and reserving Arthrosamid for patients in whom PRP results are insufficient or short-lived. This stepwise approach makes clinical sense and allows patients to benefit from a biological treatment first before moving to a more durable synthetic option.
Frequently Asked Questions
Is Arthrosamid better than PRP for knee pain?
Arthrosamid generally offers longer-lasting results and requires only one injection, while PRP uses a biological approach that many patients prefer. Neither is universally better. The right choice depends on your OA severity, budget, and previous treatment history.
How many PRP injections do you need for knee arthritis?
Most protocols involve one to three injections spaced 2–4 weeks apart. A repeat course may be needed every 12–24 months when symptoms return.
Which knee injection lasts the longest?
Based on current evidence, Arthrosamid has the longest documented duration of effect up to three years or more from a single injection. PRP typically lasts 6–24 months depending on platelet concentration and OA severity.
What are the side effects of Arthrosamid injection?
The most common side effects are mild to moderate and include temporary pain, swelling, and warmth at the injection site. These usually resolve within a few days. No serious adverse events have been reported in published clinical trials. The overall adverse event rate is around 28.9%, compared to 7.6% for hyaluronic acid.
Can PRP and Arthrosamid be used together?
There are no published trials on combining the two treatments directly. PRP combined with hyaluronic acid has shown additional benefit in some studies, but combining PRP with Arthrosamid is not yet standard practice. Speak to your specialist about a stepwise approach if one treatment has not provided sufficient relief.
How do I find a clinic offering both PRP and Arthrosamid?
Most specialist musculoskeletal and regenerative medicine clinics now offer both options. When you book a consultation to discuss PRP vs Arthrosamid injection for knee pain, ask specifically about their ultrasound guidance protocol, platelet concentration for PRP, and published outcomes for Arthrosamid. A good clinician will help you weigh both options against your specific OA grade and lifestyle.
Both PRP and Arthrosamid offer a clear upgrade from short-lived steroid injections. PRP suits patients who prefer a biological approach at a lower upfront cost, while Arthrosamid delivers single-injection, longer-lasting structural relief often making more financial sense over three years.
The right choice depends on your OA severity, budget, and treatment history. Consult an experienced orthopaedic specialist to find the path that works best for you.
Read more: Menopause and Knee Pain: Why It Happens and How to Manage It
Read more: Best Knee Pain Relief Foods to Improve Mobility and Joint Health
Read more: Arthrosamid Knee Injection Long Lasting Relief or a Permanent Solution