How Your BMI and Osteoarthritis Are Closely Connected

BMI and osteoarthritis share a relationship that most people overlook until their knees start making it impossible to ignore. As someone who has spent years helping people find clear, research-backed health information online, I find this topic both urgent and genuinely underappreciated.
Your body mass index is more than a number on a wellness chart. It reflects the pressure your joints absorb every single day. When that number climbs, your knees, hips, and even your hands start paying for it gradually, quietly, and then all at once.
What Is Osteoarthritis? Understanding Causes and Symptoms
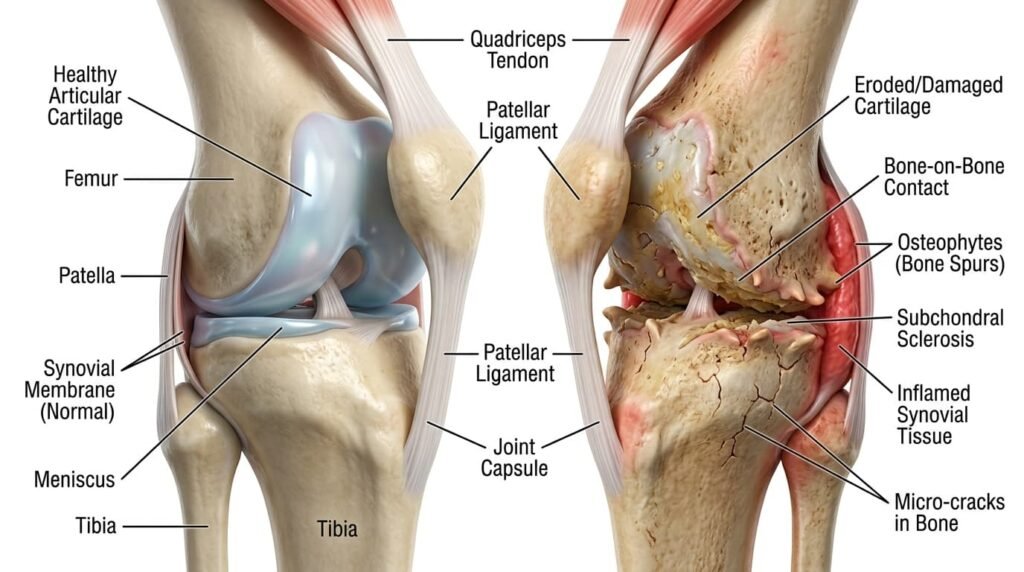
Osteoarthritis is the most common form of arthritis, affecting hundreds of millions of adults worldwide. It is a degenerative joint condition where the protective cartilage cushioning the ends of your bones gradually breaks down. Once that cushion wears thin, bone begins grinding against bone — and that’s when the pain becomes hard to dismiss.
Most people think of it as something that only affects the elderly. That’s not entirely true — and by the time symptoms appear, the damage has often been building for years.
How Joints Deteriorate — and When to Pay Attention
Osteoarthritis develops slowly. Early signs are easy to brush off as “just being a bit stiff.” Over time, they become harder to ignore. What to watch for:
- Persistent joint pain, especially after physical activity or at the end of the day
- Morning stiffness that typically eases within 30 minutes of moving around
- Swelling around the knee, hip, or finger joints
- Reduced range of motion — bending, turning, or climbing stairs feels harder than it used to
- A grating or clicking sensation in the joint during movement
The knees are the most commonly affected joints, followed by the hips, hands, and spine. Osteoarthritis risk factors include age, genetics, previous joint injuries, and physical occupation. But one of the most significant — and the most changeable — is body weight. That’s where the story really begins.
The Joint Pain and Obesity Connection
The joint pain and obesity connection is not a vague clinical suspicion. It’s backed by decades of consistent, well-documented research across large populations.
Data from the National Health and Nutrition Examination Survey found that obese women had nearly four times the risk of knee osteoarthritis compared to non-obese women. For obese men, the risk was nearly five times greater. When the numbers are that stark, they deserve more than a passing mention.
Why Obesity Becomes a Major Arthritis Risk Factor
Obesity contributes to osteoarthritis through two distinct but equally important pathways:
1. Mechanical Load on Joints
For every pound of body weight carried, the knee absorbs roughly four pounds of compressive force during walking. Going up stairs increases this further. A 20-pound weight gain translates to an extra 80 pounds of force on each knee — with every step you take. That’s not a metaphor. That’s physics working directly against your cartilage.
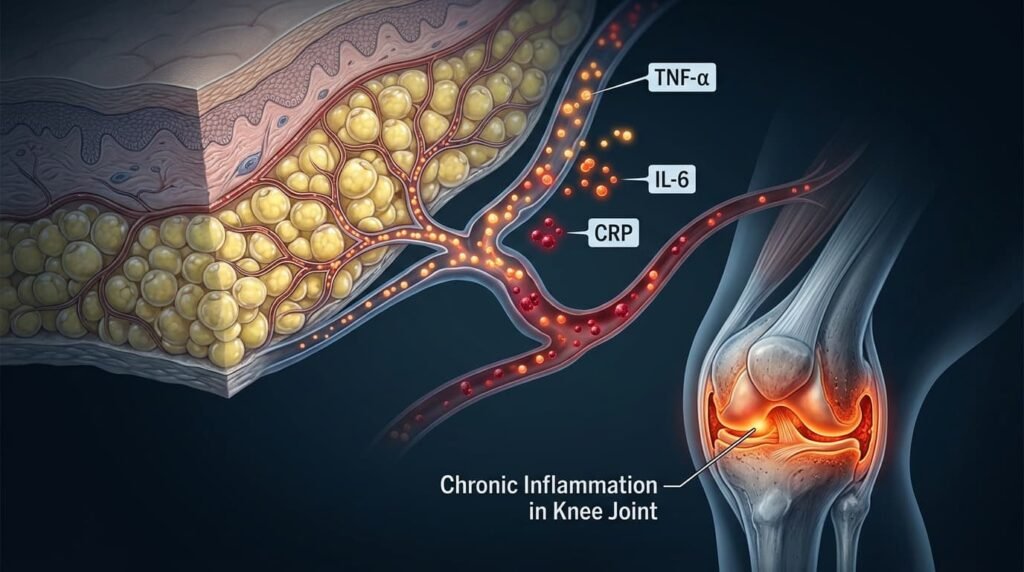
2. Systemic Inflammation from Fat Tissue
Fat tissue is not simply passive storage. It actively releases inflammatory chemicals — including interleukin-6, TNF-alpha, and C-reactive protein that speed up joint damage throughout the body. This explains why being overweight causes arthritis even in non-weight-bearing joints like the hands and fingers.
So when people ask me about overweight knee pain, my answer is always the same: it’s not just mechanical, it’s chemical, too.
3. Metabolic Syndrome and Oxidative Stress
Obesity triggers broader metabolic dysfunction. The resulting increase in oxidative stress — essentially an excess of free radicals the body can’t neutralise weakens the structural integrity of the joint from multiple angles. The synovium (the joint lining) and the subchondral bone beneath the cartilage both suffer damage, making the joint less stable and far more vulnerable to progressive deterioration.
4. Altered Biomechanics
Carrying excess body weight often changes the way a person walks subtly at first, then more noticeably. This shift in gait creates unnatural loading patterns across the joint, concentrating stress on specific areas of cartilage that weren’t built to absorb it repeatedly. The result is faster, more localised damage progression. It’s one reason why overweight knee pain often appears on just one side of the joint before spreading.
So when people ask me about the joint pain and obesity connection, my answer is always the same: it’s mechanical, chemical, metabolic, and biomechanical all at once.
BMI and Osteoarthritis — How the Numbers Stack Up
Your body mass index is calculated from your height and weight, and it is one of the clearest predictors of osteoarthritis risk in clinical research. The pattern is consistent: as BMI rises, so does the rate of joint deterioration.
For every 5 kg of weight gained, the risk of developing osteoarthritis increases by 36%. A BMI above 30 (the obese range) more than doubles the likelihood of knee OA. And the higher the BMI climbs, the faster cartilage breaks down.
The relationship between BMI and osteoarthritis doesn’t just tell us who gets the condition it predicts how quickly it will progress once it begins.
Knee Cartilage Damage from Obesity — The Mechanical Reality
Cartilage has no blood supply of its own. It absorbs nutrients through the movement and compression of the joint, which circulates fluid around it. When obesity places excessive and sustained load on a joint, the cartilage gets compressed too hard, too frequently and gradually loses its ability to recover and repair.
Understanding the direct link between BMI and osteoarthritis helps explain why cartilage loss accelerates so predictably as body weight increases.
Knee cartilage damage from obesity isn’t dramatic or sudden. It’s cumulative a slow erosion that builds over years of loading beyond what the joint was built to manage.
Knee pain from body weight is often the first signal. Many people manage it with painkillers and carry on. What I’d suggest instead: treat that signal as early, actionable information. The longer excess body weight continues pressing on weakened cartilage, the narrower your options become.
A large-scale Framingham study found that overweight adults in their thirties well before the typical age of OA onset were already at significantly elevated risk for knee osteoarthritis in later decades. The damage timeline starts earlier than most people expect.
Does Losing Weight Help Arthritis?
Does losing weight help arthritis? The research answer is a clear, well-documented yes.
A meta-analysis of randomised controlled trials found that a body weight loss of just 5.1% at a rate of approximately 0.24% per week produces clinically meaningful improvements in knee pain and physical function. That’s not a dramatic number. It’s an achievable one.
And when you understand what we know about BMI and osteoarthritis progression, even modest weight reduction starts to make mechanical sense: less weight, less force, less cartilage stress.
How Much Weight Loss Actually Reduces Knee Pain
If you’re wondering about how much weight loss to reduce knee pain, here’s one number worth remembering: for every pound of body weight lost, the load on each knee during walking drops by four pounds.
Lose 10 pounds. Your knee absorbs 40 fewer pounds of force with every step. Over a full day of walking, that adds up to an enormous reduction in cumulative joint stress.
Research also shows that a 10% reduction in body weight improves joint pain, physical function, and overall quality of life while simultaneously lowering systemic inflammation. Greater weight loss produces greater results. The pattern is consistent.
Can Weight Loss Reverse Osteoarthritis?
Here’s where honesty matters more than optimism. Can weight loss reverse osteoarthritis? Not entirely.
Once cartilage has been lost, weight loss cannot rebuild it. But it can do a great deal of other things:
- Slow or stop further cartilage deterioration
- Reduce daily pain levels significantly
- Delay or potentially eliminate the need for knee replacement surgery
- Restore meaningful mobility and independence in daily life
Think of it as stopping a slow structural leak rather than undoing years of damage overnight. The outcome is still genuinely worthwhile especially for those losing weight with knee arthritis, where even modest reductions bring tangible relief that keeps motivation going.
Osteoarthritis Weight Management — Diet and Exercise That Work
Sustainable BMI and osteoarthritis weight management doesn’t require extreme dieting or high-intensity gym sessions. It requires consistency, the right food choices, and physical movement your joints can actually handle.

Best Diet for Knee Osteoarthritis
The best diet for knee osteoarthritis is one that reduces inflammation while supporting a healthy body weight. Those two goals overlap more than most people expect and hitting both at once is entirely realistic.
An anti-inflammatory diet for arthritis typically prioritises:
Eat More Of:
- Fatty fish (salmon, mackerel, sardines) — rich in omega-3 fatty acids proven to reduce joint inflammation
- Colourful vegetables and fruits — packed with antioxidants that reduce oxidative stress in joint tissue
- Extra-virgin olive oil — contains oleocanthal, a natural compound with anti-inflammatory properties comparable to low-dose ibuprofen
- Whole grains (oats, quinoa, brown rice) — support gut health and help maintain steady body weight over time
- Legumes and lentils — excellent lean protein sources with additional anti-inflammatory benefits
Eat Less Of:
- Refined sugars and processed carbohydrates
- Red and processed meats
- Fried foods and trans fats
- Excessive alcohol
This isn’t about removing all joy from mealtimes. An anti-inflammatory eating approach simply means choosing foods that work with your body rather than against your joints. And for the record salmon with olive oil actually tastes good. That’s a free win.
Low Impact Exercise for Knee Arthritis — What Actually Works
Exercise for BMI and osteoarthritis overweight people with knee pain has to be joint-conscious. The goal is building muscle strength and burning calories without stacking additional stress onto already-damaged cartilage.

My top recommendations for low impact exercise for knee arthritis:
- Swimming and water aerobics — water’s buoyancy removes impact entirely while engaging the whole body
- Stationary or outdoor cycling — builds quadricep strength without compressing the knee joint
- Flat-surface walking — widely accessible, costs nothing, and most OA patients can start today
- Chair yoga and gentle stretching — improves flexibility and reduces morning joint stiffness
- Resistance band exercises — strengthens the hip and thigh muscles that stabilise and protect the knee
Start with 10–15 minute sessions. Build gradually. The American College of Rheumatology recommends a combination of aerobic and resistance exercise for OA management — and the clinical evidence supports both types consistently.
Weight loss joint pain relief is not a passive outcome. It requires consistent movement but the kind of movement that’s sustainable and actually achievable week after week.
What You Can Do About It — A Practical Action Plan
Knowing the cause is one thing. Having a clear plan is another. Here’s what I’d actually recommend if you’re managing osteoarthritis weight management alongside daily joint pain:
- Target 10–20% weight loss. Losing 10–20% of your body weight has been shown to significantly reduce joint pain and improve physical function. You don’t need to reach an “ideal” BMI even getting partway there produces measurable relief. Start with a 5–10% goal and build from it.
- Commit to 150 minutes of low-impact aerobic activity per week. Walking, cycling, and swimming all count. Combine these with strength training two to three times a week to support the muscles that stabilise the knee. More muscle around the joint means less strain on the cartilage.
- Eat to reduce body fat and inflammation together. Follow a whole-food, anti-inflammatory eating plan that creates a modest calorie deficit without cutting out nutrients your joints need. Crash diets are not the answer here — slow, steady fat loss through healthy nutrition is.
- Use support tools on difficult days. Cushioned footwear, a knee brace, or a walking stick can reduce daily joint impact considerably. These aren’t signs of giving up — they’re practical ways to stay active while the weight comes down gradually.
- Work with a physiotherapist. A physiotherapist can design a programme that strengthens the specific muscles around your knee, improves joint stability, and corrects any movement patterns that may be accelerating damage. This is especially useful if altered gait has become part of the picture.
None of these steps require a dramatic lifestyle overhaul overnight. Small, consistent changes applied across all five areas compound over time into real, lasting improvement.
FAQ
Can osteoarthritis develop in younger adults who are overweight?
Yes. The Framingham study found that overweight adults in their thirties were already at significantly higher risk of developing knee osteoarthritis in later decades — well before the typical age of onset. Excess body weight creates cumulative joint damage long before any pain or stiffness becomes obvious.
Are medications effective for managing OA alongside weight loss?
Anti-inflammatory medications (NSAIDs), topical treatments, and corticosteroid injections can help manage OA pain. More recently, GLP-1 receptor agonists such as semaglutide have shown potential for both significant weight loss and OA symptom improvement. Medication works best when paired with sustained lifestyle changes rather than used alone.
Does vitamin D deficiency affect osteoarthritis?
Yes. Vitamin D deficiency is common among OA patients and can worsen symptoms over time. Adequate vitamin D levels support bone density and may help reduce inflammation around joints. A simple blood test is the most reliable way to check your current levels. Speak with your doctor before starting any supplementation.
How does bariatric surgery relate to OA outcomes?
Research shows that bariatric surgery — which produces substantial, sustained weight loss — can significantly reduce knee OA symptoms and lower the risk of needing knee replacement surgery. It is not a first-line treatment, but for individuals with severe obesity and advanced OA, the outcomes can be substantial and life-changing.
Is it safe to exercise daily with knee osteoarthritis?
For most people with OA, daily low-impact activity is not only safe — it’s recommended. The important thing is avoiding high-impact activities like running, jumping, or heavy squats, and choosing joint-friendly movement instead. Start gradually and build up. Always check with your doctor or physiotherapist before beginning a new exercise programme, especially if your OA is moderate to severe.
Does poor sleep quality affect osteoarthritis progression?
Emerging research links consistently poor sleep with increased pain sensitivity and slower physical recovery in OA patients. While sleep is not a direct cause of OA, chronic poor sleep can make pain harder to manage and reduce the motivation to exercise or maintain dietary changes — both of which matter considerably in long-term weight management and joint health.
The link between BMI and osteoarthritis is one of the clearest in joint health research — and one of the most actionable. Your body weight doesn’t just affect your energy levels or how your clothes fit. It directly shapes how your joints function, how fast they deteriorate, and how much pain you manage on a daily basis.
The encouraging reality is that you don’t need a dramatic transformation to feel a real difference. Modest, consistent progress a few pounds at a time, smarter food choices, and movement your joints can actually handle adds up to genuine, lasting improvement.
Read more: Overweight Knee Pain Relief for Arthritis and Joint Health
Read more: Best Knee Pain Relief Foods to Improve Mobility and Joint Health